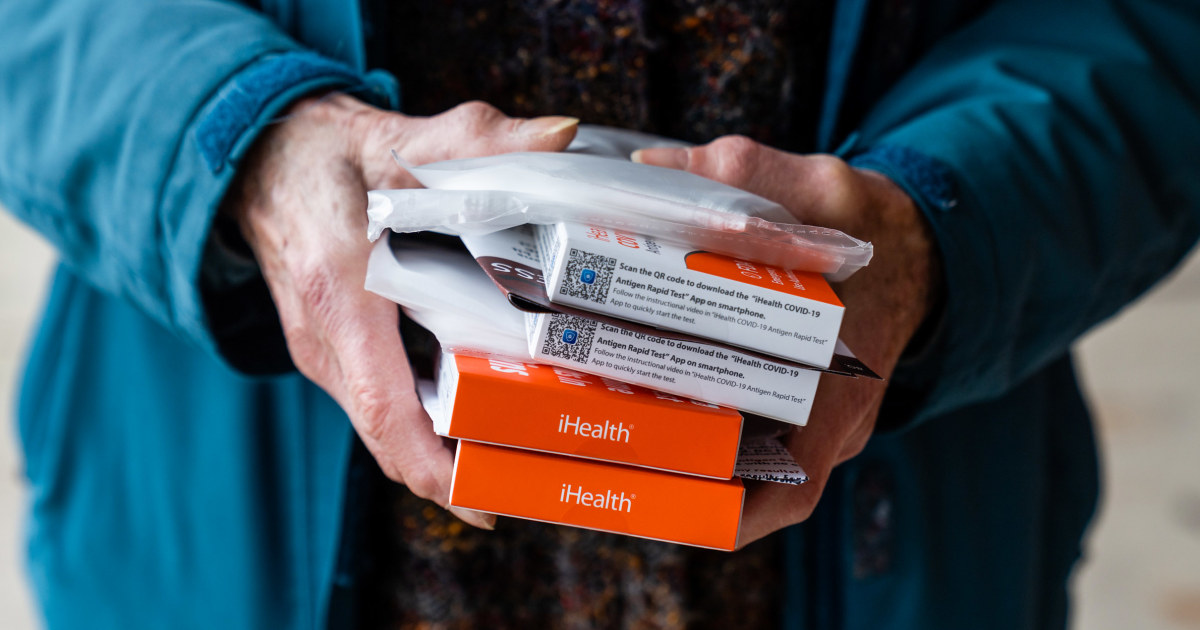
Most people can expect to pay more for covid tests after the federal public health emergency expires at the end of the day Thursday.
The emergency declaration guaranteed widespread access to free Covid-related health services from January 2020.
But once it ends, people with employer-based private health insurance could start paying for home covid tests, as well as rapid or lab tests at a doctor’s office or clinic. Several large insurance companies, including UnitedHealthcare, Cigna and Aetna — have said that their home testing coverage, which costs about $11 on averageIt will end on Thursday.
In California, however, residents will have continued access to free tests, vaccinations and treatments provided by licensed healthcare providers through November 11.
Additionally, the US government is distributing free home tests of the National Stock through the end of the month. He The Department of Health and Human Services said Tuesday that the government could decide to send more tests in the future depending on the supply.
Federally purchased doses of Paxlovid, the gold standard treatment for people at risk of severe disease, could also remain free while supplies last. according to KFFa non-profit group of health experts.
These are the expected changes in costs related to Covid.
The tests will be more expensive
- For people with private insurance: Insurers will no longer pay for up to eight free home tests per month. Rapid or laboratory tests ordered or administered by a physician will be fully covered but subject to the individual’s plan, so individuals may be responsible for deductibles or copays. Insurers may also limit the number of tests covered per person or require a prior authorization process.
- For those with Medicare: People will no longer receive up to eight home covid tests per month covered, but lab tests ordered by a doctor or other health care provider will be at no out-of-pocket cost. Some people with Medicare Advantage may continue to get home testing coverage under their plans, but may incur costs for PCR or antigen tests.
- For those with Medicaid: States must provide coverage for covid tests of all types through September 30, 2024. After that, coverage may vary by state.
- For people without insurance: During the public health emergency, 18 US states and territories covered the costs of Covid testing for the uninsured through Medicaid. That ends Thursday, though people without insurance can still find free tests through some community clinics.
Vaccines will largely continue to be covered
- Private insurance: Vaccines and boosters will continue to be covered if administered by an in-network health care provider. However, individuals may be charged if they are vaccinated by an out-of-network provider.
- State health insurance: Vaccines will remain covered if the patient’s doctor or health care provider agrees to be paid directly by Medicare. Those with Medicare Advantage will also not be charged if they use an in-network provider.
- Health insurance: States must provide coverage without cost-sharing through September 30, 2024. After that, Medicaid will likely continue to cover the cost of vaccines.
- Uninsured: Medicaid coverage for vaccines will end in 18 states and US territories, but a hhs program make sure vaccines stay free to those without insurance.
Treatment costs will vary depending on the type of insurance
- Private insurance: The federal government ordered and paid for a reserve of Paxlovid, so many patients have so far received the antiviral for free, regardless of their insurance type. That will remain true for the duration of the reserve, but after that, Paxlovid costs will be subject to an individual’s insurance plan, so individuals may incur co-pays or out-of-pocket costs. Insurers are not required to waive out-of-pocket costs for Covid treatment, such as antiviral pills, doctor visits, or hospital care. Some did it voluntarily during the public health emergency, though most insurers stopped covering treatment costs by 2021.
- State health insurance: Deductibles and out-of-pocket costs for treatment will remain the same for people with traditional Medicare, but Medicare Advantage may require patients to see in-network providers for treatment to be covered. Paxlovid will remain free while the federal supply lasts, although people with Medicare Part D can get the drug at no out-of-pocket cost until December 2024.
- Health insurance: States must provide coverage for Covid treatment through September 30, 2024. After that, coverage may vary by state.
- Uninsured: Medicaid coverage for testing will end in 18 US states and territories, but HHS will make sure people without insurance don’t pay out-of-pocket for certain drugs like Paxlovid or Lagevrio (another oral antiviral). However, individuals may still be responsible for hospital fees or doctor visits for treatment.